Bangkok Hospital Pattaya was established on 23 June 1990 in Pattaya, Chonburi Province, one of Thailand’s leading seaside destinations on the Eastern Seaboard.
As part of Bangkok Dusit Medical Services (BDMS), the hospital serves as a major referral center for the Eastern region of Thailand. Since its establishment, the hospital has grown into a 300-bed tertiary care facility providing comprehensive diagnostic, treatment, and rehabilitation services. Bangkok Hospital Pattaya is recognized as a center of specialized healthcare, supported by more than 100 full-time specialists and advanced medical technology, including Digital MRI 3.0 Tesla, 128-slice CT Scan, OCT retinal imaging, PACS, and fully integrated electronic medical records. Key centers of excellence include the Heart Center, Neuroscience Center, Emergency Medical Service Center, Orthopedic Center. The Heart Center is equipped with advanced cardiac diagnostic and interventional technologies, including catheterization laboratories, electrophysiological studies, Extracorporeal Membrane Oxygenation (ECMO) and minimally invasive cardiac procedures, comparable to leading hospitals in Bangkok. To enhance patient comfort and service capacity, the hospital expanded from 5 to 9 acres, including the addition of a 15-storey building in 2006. Today, Bangkok Hospital Pattaya serves both Thai and international patients, with approximately 40% of patients coming from overseas. Interpreter services are available in more than 20 languages, supported by staff trained in international communication and cultural understanding. Bangkok Hospital Pattaya has maintained a strong commitment to quality and international standards. The hospital has received multiple Hospital Management Asia (HMA) Awards and Value Based Healthcare Prize (VBHC). It was first accredited by Joint Commission International (JCI) in 2009 and has successfully maintained subsequent re-accreditations, reflecting consistent excellence in patient safety and clinical quality. In line with its commitment to value-based healthcare, the hospital is also accredited by the International Consortium for Health Outcomes Measurement (ICHOM). Bangkok Hospital Pattaya is the first hospital in Thailand for accreditation Level 1 to achieved ICHOM certification for Coronary Artery Disease and Stroke, expanded to Heart Failure and Diabetes, and in 2025 became the first hospital in Thailand to receive ICHOM Level 2 Accreditation for Coronary Heart Disease and Stroke. Through continuous innovation, international accreditation, and patient-centered care, Bangkok Hospital Pattaya remains dedicated to delivering world-class healthcare and strengthening its position as one of the leading hospitals in Thailand and Southeast Asia.

ICHOM Accreditations




Patient Impact
(Click on each for detail)
Cardiovascular Center – Acute Coronary Syndrome (ACS)
A 50-year-old Indian man working in Rayong Province presented with acute chest pain and was initially admitted to a local hospital, where electrocardiography confirmed NSTEMI. After receiving primary treatment, he was referred to Bangkok Hospital Pattaya (BPH) for advanced care.
Coronary angiography at BPH revealed Three-Vessel Disease (TVD), and the patient underwent successful coronary artery bypass graft surgery (CABG). While the immediate surgical outcome was favorable, a key patient-centered question remained
Would he be able to return to his normal life and work?
Using ICHOM to Look Beyond Clinical Outcomes
To address this question, the multidisciplinary team applied the ICHOM ACS framework to systematically monitor post-treatment outcomes beyond conventional clinical indicators.
At the one-month post-operative assessment, the patient reported:
“I still don’t feel ready to return to work.”
Although clinical parameters suggested satisfactory recovery, ICHOM outcome assessment revealed that the patient still had unmet functional and recovery needs, highlighting significant potential for further improvement.
ICHOM-Driven Change in Care
Based on the ICHOM assessment, the care plan was individually adjusted:
- Nutritional assessment identified inadequate protein intake; targeted nutritional therapy was initiated.
- Continuous monitoring and follow-up were provided through Telehealth services.
- The patient’s wife was actively involved in rehabilitation, receiving exercise guidance via Tele Line OA.
- Physical recovery was objectively monitored using cardiopulmonary exercise testing (CPET) and functional capacity assessment at the 5-METs level.
Patient-Meaningful Outcomes
After one additional month of targeted intervention and close follow-up, the patient demonstrated marked functional improvement and successfully returned to work.
The patient reflected:
“Thank you to the care team for helping me return to work. It feels as if I never had heart disease.”
The transformation was evident. Initially requiring a wheelchair, the patient progressed to independent daily activities within two months and resumed regular exercise, including running.
Restoration of Life Goals
The patient’s personal goal extended beyond returning to work:
“I want to go mountain climbing again.”
Based on the most recent CPET results, the multidisciplinary team confirmed that his physical condition was sufficient to safely pursue this activity.
Conclusion
This case demonstrates that ICHOM is not merely a tool for outcome measurement, but a structured approach that translates patient-reported outcomes into meaningful care adjustments. By aligning clinical decisions with what truly mattered to the patient, the ICHOM framework supported recovery from uncertainty to restored function, renewed confidence, and the ability to return to a life the patient values.
Cardiovascular Center – Heart Failure & Valvular Heart Disease
A 76-year-old foreign male with a known history of heart failure and severe aortic stenosis was admitted with progressive dyspnea and chest tightness. Initial clinical evaluation indicated acute myocardial ischemia. Coronary angiography revealed significant coronary artery stenosis, and the patient underwent percutaneous coronary intervention (PCI).
Following PCI, the patient’s clinical symptoms and conventional medical indicators showed clear improvement. However, the multidisciplinary team applied the ICHOM framework to assess outcomes that reflected the patient’s functional status and quality of life.
When Clinical Improvement Was Not Enough
Despite apparent clinical success, follow-up ICHOM outcome assessments demonstrated that the patient’s ROSE Dyspnea Score and EQ-5D (EuroQol) scores had not meaningfully improved compared to baseline. These results indicated that, from the patient’s perspective, daily function and quality of life remained significantly limited.
This discrepancy prompted the care team to recognize that additional factors were contributing to the patient’s ongoing limitations.
ICHOM-Guided Clinical Decision-Making
In response to the outcome data, a comprehensive reassessment was undertaken. Further evaluation, including echocardiography, confirmed persistent severe aortic valve stenosis, which was identified as the primary driver of the patient’s reduced functional capacity and quality of life.
Based on these findings, the multidisciplinary team made a shared decision to proceed with Transcatheter Aortic Valve Implantation (TAVI), aligning the treatment plan with the patient’s unmet functional goals.
Meaningful Outcomes After Targeted Intervention
Following TAVI and continuous follow-up, the patient demonstrated substantial improvement in outcomes that mattered most to him. ICHOM assessments showed marked improvement, particularly in dyspnea and overall quality of life.
The patient reflected on his experience:
“My condition has improved greatly. If I had to give a score, it would be 100%. I am not disappointed at all that I chose to receive treatment here.”
Conclusion
This case illustrates that ICHOM is not merely an outcome measurement tool, but a decision-support framework that guides care teams toward interventions that truly improve patients’ lives. By revealing gaps between clinical indicators and patient-reported outcomes, ICHOM helped bridge the divide between treatment that appeared successful and care that genuinely restored the patient’s quality of life and functional independence.
Recovery Beyond Clinical Outcomes.
A 67-year-old Thai woman was admitted with acute left-sided weakness and balance impairment and was diagnosed with ischemic stroke. Prior to her illness, she was fully independent, actively caring for her family, and valued her personal confidence and self-identity.
During hospitalization, the patient expressed a key personal concern — her fear of losing independence and no longer being able to walk confidently, including wearing high-heeled shoes, which she associated with her sense of self and dignity.
“I was afraid I wouldn’t be able to walk confidently again or be myself.”
Her concerns and personal goals were actively incorporated into multidisciplinary care planning. The rehabilitation team used her stated priorities to guide physical and occupational therapy goals, ensuring that treatment focused not only on functional recovery, but also on what mattered most to the patient.
Rehabilitation progressed step by step, with continuous encouragement and adjustment based on the patient’s functional ability and confidence. The patient actively participated in her recovery process, including practicing balance and walking skills aligned with her personal goals.
At discharge, the patient was able to walk independently and reported restored confidence in daily activities. She returned home with improved functional status and quality of life.
This case demonstrates how patient-reported goals and values were integrated into clinical decision-making, supporting recovery that addressed both physical function and personal dignity — a core principle of value-based, patient-centered care.

At Bangkok Hospital Pattaya, our partnership with ICHOM has been instrumental in transforming care for Coronary Artery Disease and Stroke through a truly value-based, patient-centred approach. By adopting ICHOM’s standardized outcome frameworks, tools, and global best practices, we moved beyond provider-focused metrics to systematically measure outcomes that matter most to patients, including quality of life, functional recovery, and return to independence. In Coronary Artery Disease, this approach has delivered strong clinical and patient- reported outcomes, with a 97% first-year survival rate, a repeat surgery rate reduced to 2%, and 88% of patients returning to daily activities or work within three months. In Stroke care, the proportion of patients able to live independently at 90 days rose to 93%, while quality-of-life scores reached 95% and length of stay continued to decline. Achieving the world’s first ICHOM Level 2 certification in both Coronary Artery Disease and Stroke reflects the greatest impact of our partnership: aligning multidisciplinary teams around standardized outcomes to deliver measurable, meaningful, and sustainable value for patients and stakeholders alike."
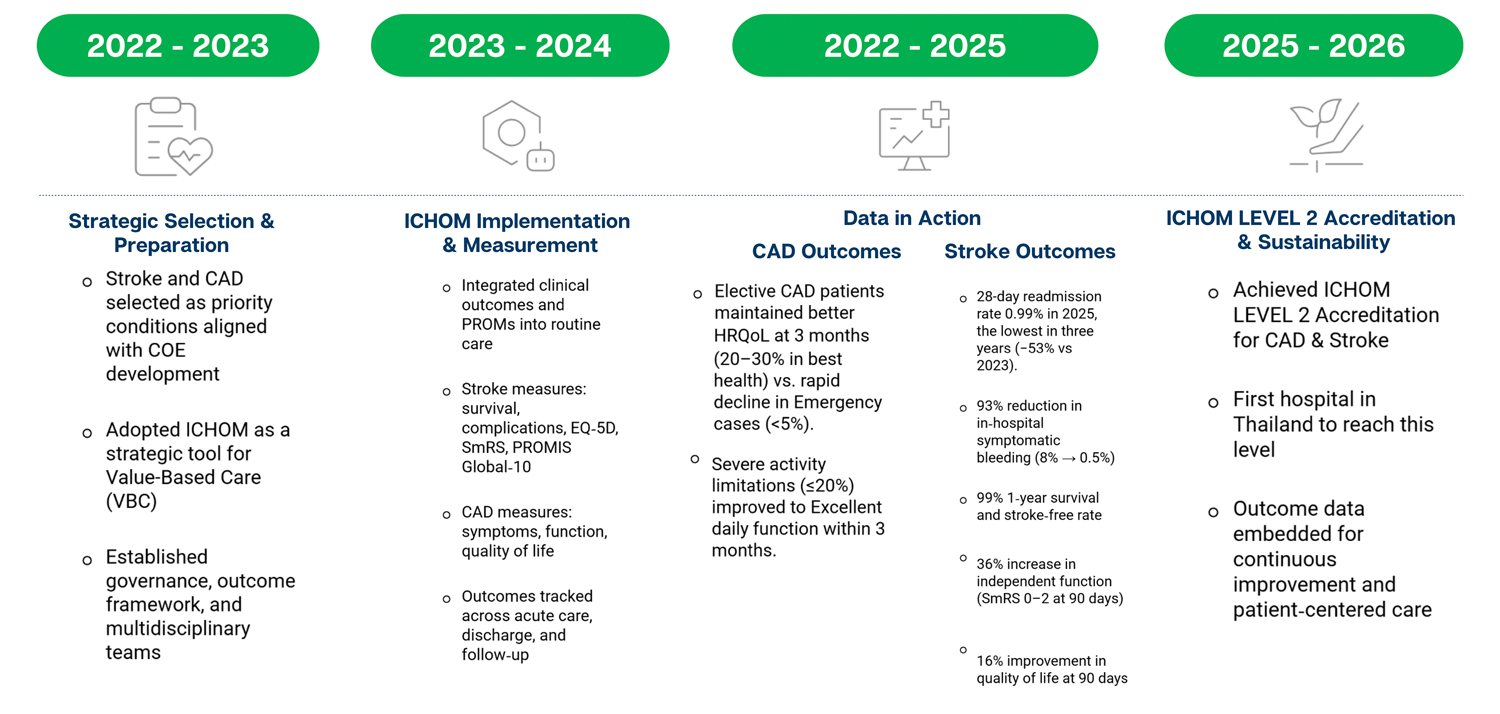
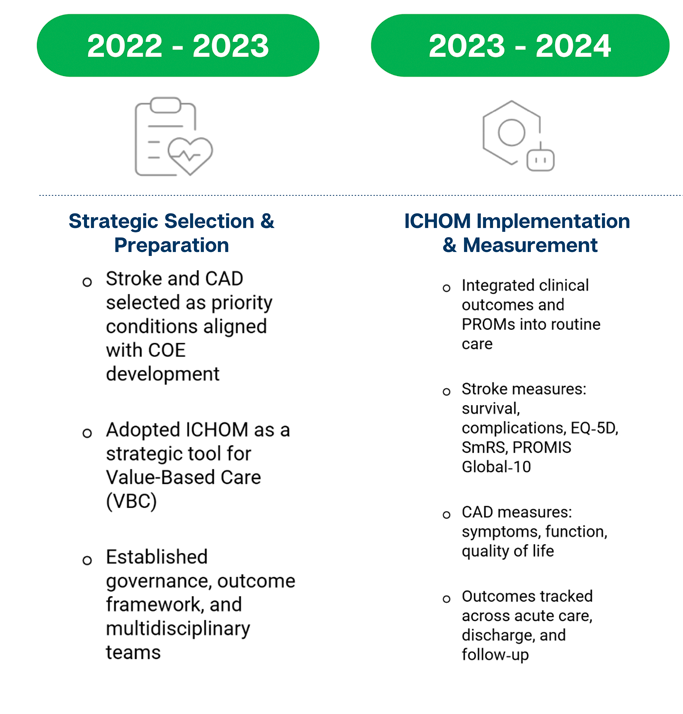
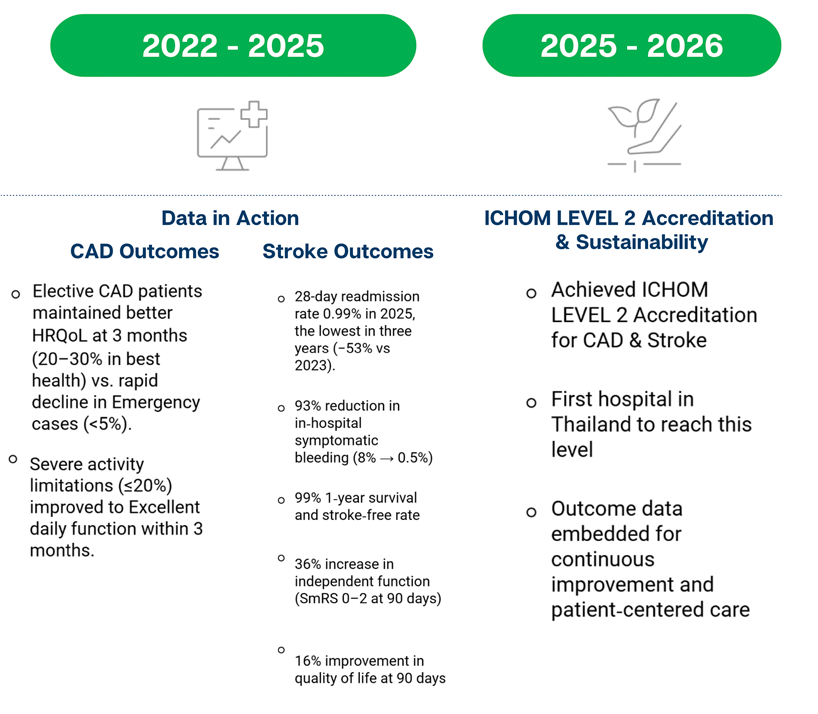
ICHOM LEVEL 2 Accreditation Journey
Coronary Artery Disease & Stroke Bangkok Hospital Pattaya